 
A baseline measurement of pupil size should be made under ambient lighting conditions with both pupils equally illuminated. Any asymmetry of the colour of the two irides (heterochromia) should be noted. The examiner should observe the shape, size and location of the patient’s pupil. Testing this forms the basis of the swinging-torch test: if the response to shining a light in one eye differs from shining it in the other, this is referred to as a relative afferent pupillary defect (RAPD). 2,5ĭirect and consensual responses should be identical, whichever eye is illuminated. 2,5 Third-order sympathetic neurons then travel to the orbit with the internal carotid artery and its branches, ultimately innervating the dilator pupillae muscle in the iris. 5 From here, second-order sympathetic neurons travel back up the sympathetic chain to synapse in the superior cervical (stellate) ganglion. 2 Sympathetic pupillary fibres originate in the hypothalamus, travel down the brainstem and cervical spinal cord to exit at the first thoracic level. Parasympathetic pupilloconstrictor fibres travel in the oculomotor nerve, synapsing in the ciliary ganglion before reaching the sphincter pupillae muscle in the iris. 5 It is this bilateral innervation of the Edinger-Westphal nucleus that results in both direct and consensual responses to light shone in one eye. 2 Information from the optic nerve passes to the ipsilateral pretectal nucleus and then on to the Edinger-Westphal nuclei on both sides. The pupillary light response involves both afferent (optic nerve) and efferent (oculomotor nerve and sympathetic) pathways. Examination should include assessment of visual acuity, visual fields to confrontation, pupil testing, extraocular motility and whether or not ptosis is present. 5 It is important to ask about previous or current malignancies and neck trauma. Associated visual and/or neurological symptoms should be sought, including visual blurring, visual loss, disturbance of visual fields, or diplopia. 2,5Ī thorough history should include asking about the use of new medications or inadvertent ocular contact with foreign substances by rubbing the eyes. 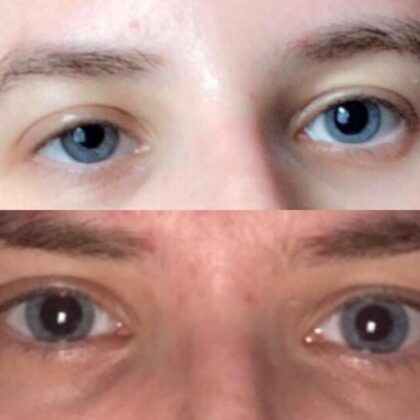
2–4 Non-physiological anisocoria indicates disease of the sympathetic or parasympathetic pathways supplying the pupil, or a problem with the iris itself. Physiological anisocoria is common: approximately 20% of normal people have different-sized pupils. 1 This article aims to guide management in both of these situations. Indeed, new onset anisocoria may be an early sign of a life-threatening emergency. The general practitioner (GP) may discover anisocoria during examination for a seemingly unrelated problem. The aetiology may be physiological, pathological or pharmacological. 2003 110(8):1606-14.Īmerican Academy of Ophthalmology.A difference in pupil size between the eyes is known as anisocoria. Pupil size and quality of vision after LASIK. 
Schallhorn SC, Kaupp SE, Tanzer DJ, Tidwell J, Laurent J, Bourque LB. Ocular manifestations of drug and alcohol abuse. Pupillary reactivity as an early indicator of increased intracranial pressure: the introduction of the Neurological Pupil index. doi:10.3892/ol.2017.5648Ĭhen JW, Gombart ZJ, Rogers S, Gardiner SK, Cecil S, Bullock RM. 
Iris metastasis as the first sign of small cell lung cancer: a case report. March 23, 2016.īrigham And Women's Hospital. Pupillary disorders including anisocoria.Īmerican Academy of Ophthalmology. What kinds of eye examinations are there? April 20, 2016. Anisocoria and an array of neurologic symptoms in an adult with Ewing sarcoma. Safe and sensible preprocessing and baseline correction of pupil-size data. Mathôt S, Fabius J, Van Heusden E, Van der Stigchel S. A model of the entrance pupil of the human eye. 
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
